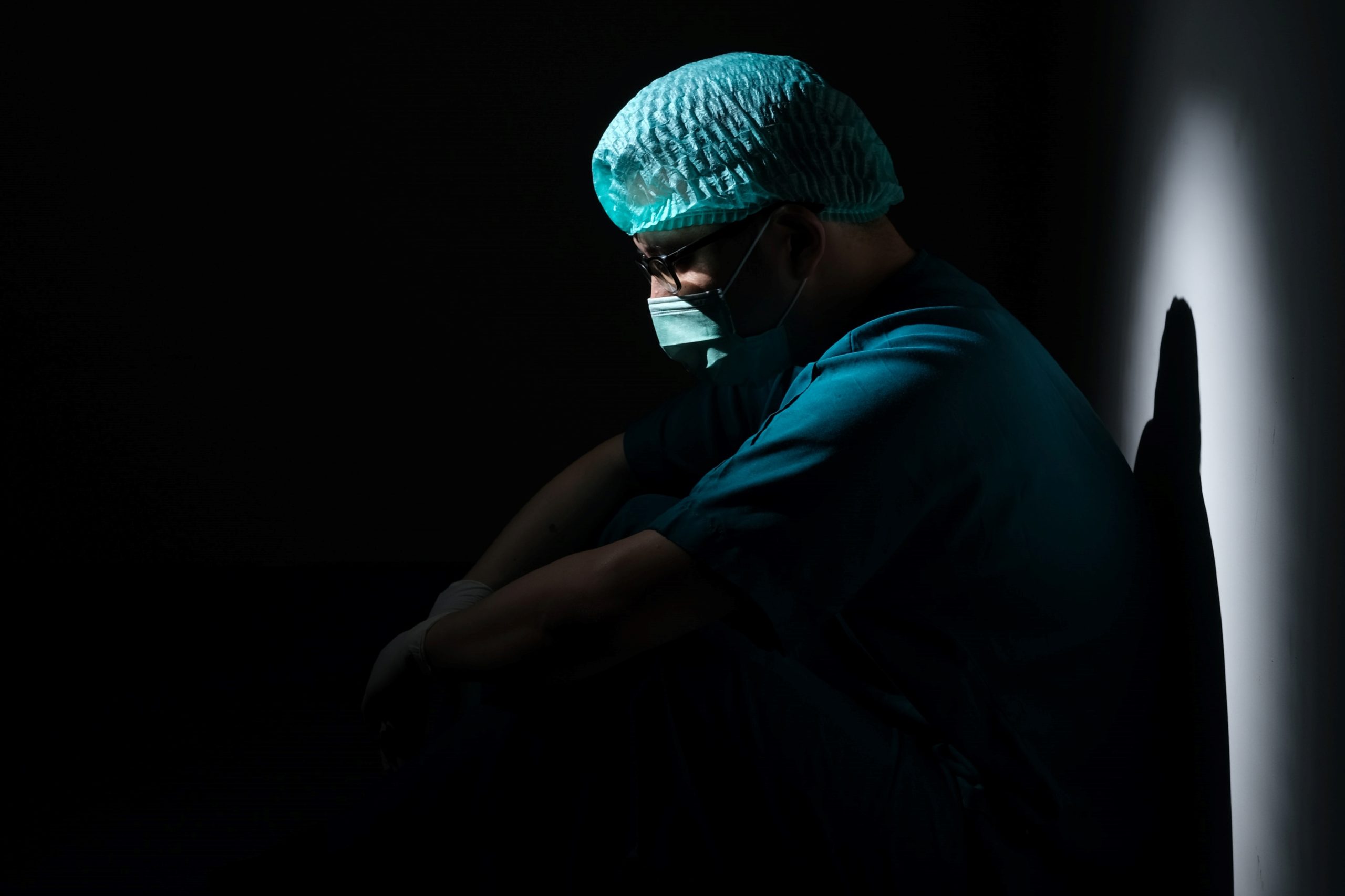
A little over a year ago, when the pandemic was threatening to take hold in our country, we watched in horror as the average number of deaths per day from COVID-19 in Italy, the epicenter of the disease in the world up to that time, was high. The sum totaled around 800 people. Today in Brazil, however, where the pandemic still seems far from being under control, the average daily death rate has been around two thousand for many months. The total number of deaths has reached five thousand, passed through four and, with considerable frequency, is again around three thousand.
Equally frighteningly, the steadily increasing number of deaths from the coronavirus seems to have been accompanied by a dampening of Brazilians’ capacity to be impressed by them. What could have happened? If, on the one hand, the explanations about the reasons that led (and continue to lead) to the mass deaths seem increasingly clear, it is not possible to say the same about the indifference and trivialization that accompany the way we have collectively dealt with them.
Focusing on this challenging and painful scenario, a group of professors and students from the Biomedical Institute, the Institute of Humanities and Health (Rio das Ostras Campus), and the Antônio Pedro University Hospital (HUAP) at UFF, as well as professors and students from four other public universities (UERJ, UNIRIO, UFRJ, and UFOP), developed a project that alerts about the urgency of looking carefully at these deaths and insists on the need to break the silencing around them. The team – which has worked together for 20 years studying mental disorders, especially Post-Traumatic Stress Disorder in different clinical and non-clinical populations – is multidisciplinary and involves researchers from the neurosciences, psychology, psychiatry, and epidemiology, among other areas.
By identifying factors that can aggravate or minimize the mental illness of these professionals, we are offering important information to the managers of hospital environments and the health system as a whole, which can be used to reduce the impact of this moment on the mental health of these individuals.
Mirtes Garcia Pereira, professor at the Biomedical Institute
and one of the coordinators of PSIcovidA.
Inaugurated in 2020, at the peak of the pandemic in the country, PSIcovidA, which is coordinated by UFF and aims to investigate the mental health of health professionals throughout this period, seeks to make visible the pain of people who have lived with these thousands of invisible deaths. More specifically, the goal is to understand the effects of Post Traumatic Stress Disorder and depression on those who worked (or continue to work) in hospital environments and in emergency care units during the pandemic. So far, according to Letícia de Oliveira, a professor at the Biomedical Institute and one of the project’s coordinators, the study has covered more than a thousand professionals in nursing, medicine, physiotherapy, psychology, and technicians from public and private institutions.
The research, which has a “longitudinal” character, i.e., it followed the evolution of clinical symptoms in at least three different moments, was developed from an online form answered by health professionals. Based on this instrument, various information about them was collected, and evaluations were also carried out to assess symptoms of Post-Traumatic Stress Disorder (PTSD) and depression.
The coordinator informs that, among the results obtained, there is, for example, greater symptomatology for these disorders among women, younger people, and also those with a technical level, and nursing assistants. In addition, those who did not have adequate access to Personal Protection Equipment (PPE) presented greater symptoms. Another aspect that draws attention is a lower severity rate among those who felt more valued professionally, especially after the pandemic began.
According to Leticia, the moment of contact with the professionals’ testimonies is sometimes very emotional, in proportion to the countless dramatic situations they experienced. “We know that these people are facing extreme conditions, such as experiencing an expressive number of deaths in a short period of time, the constant concern with the daily risk of contaminating other people or contracting the virus, excessive working hours, shortage of PPE, lack of training, choosing which patients ‘should’ receive treatment, among other surreal situations.”
The authorities need to develop policies based on evidence from those who study and know more about the topic in question. In the case of PSIcovidA, we point out fundamental factors to protect the mental health of the professionals who are in direct confrontation with the pandemic.
Letícia de Oliveira, a professor at the Biomedical
Institute and one of the project’s coordinators.
Professor Mirtes Garcia Pereira, from the Department of Physiology and Pharmacology of the Biomedical Institute, who also coordinates the project, emphasizes the exceptionality of the potentially traumatic situations experienced by health professionals. According to her, “it is already known that one of the most drastic sequels of exposure to traumatic events is the development of PTSD, which is incapacitating and brings a lot of suffering. Not all people who experience a traumatic event develop PTSD, and knowing the factors that lead to a greater susceptibility to the development of this mental illness or that provide protection against it is fundamental. By knowing the risk and protection factors, this information can be used to implement measures to prevent these professionals from getting sick”.
In addition, Mirtes highlights the importance not only of health professionals knowing about the existence of initiatives like PSIcovidA, which are attentive to their suffering but also for the population to know that they are exhausted and becoming mentally ill. The researcher states that “by identifying factors that can aggravate or minimize the mental illness of these professionals, we are offering important information to the managers of hospital environments and the health system as a whole, which can be used to reduce the impact of this moment in the mental health of these individuals. Moreover, each of us can contribute. Taking the vaccine when it’s your turn, social distancing, and wearing a mask are measures that reduce the spread of the virus and avoid overloading the hospital system, which goes hand in hand with many potentially traumatic events that these professionals are facing.”
Committed to life and science, professor Letícia de Oliveira insists on the importance of talking about this pain to which we already seem desensitized: “we need to shed light on the suffering of these professionals. It is a very serious disease. How many deaths would have been avoided if we had faced the situation with the necessary seriousness? Brazil is currently the world epicenter of the pandemic, representing 2.7% of the world’s population and 12.9% of the world’s deaths due to COVID-19. There are excess deaths in our country, avoidable deaths if our actions were minimally adequate. In addition, the mental health sequelae, not only in health professionals but in the entire population will be immense. We have to start mapping the dimension of the problem in order to draw strategies to confront it.
Letícia concludes by pointing out the public university as fundamental in this process: “it is essential for the generation of qualified knowledge that points out and details the difficulties of this reality, as well as possible solutions. The public power needs to develop policies based on evidence from those who study and know more about the topic in question. In the case of PSIcovidA, we point out fundamental factors to protect the mental health of the professionals who are in direct confrontation with the pandemic. For example, adequate supply of PPE, training for the younger ones and valuing these professionals. Those who feel recognized by the institutions in which they work, and who receive good salaries and adequate working conditions are less likely to present severe symptoms of mental disorders. On behalf of the whole team, I would like to thank each one of these wonderful professionals who have done so much at this critical time. Thank you so much!”.